The 7 Data Streams Every Nursing Home Case Requires - And Why Manual Review Takes Days

Unlike a car accident with a clear before-and-after, or a surgical error with a discrete operative report, nursing home cases unfold across weeks or months. They're documented in thousands of pages spread across multiple systems, formats, and documentation types. And the key to understanding whether negligence occurred lies not in any single document, but in the patterns that emerge when you correlate multiple data streams over time.
This is why nursing home case review is so time-consuming. And this is why generic legal AI tools - built for simpler, event-based cases - consistently fall short.
Let's break down the seven critical data streams that every thorough nursing home case analysis requires, and why connecting them is where the real investigative work happens.
1. Vital Signs: The Body's Warning System
What it includes: Temperature, blood pressure, heart rate, respiratory rate, oxygen saturation
Why it matters: Vital signs are your early warning system for developing complications. A rising temperature over several days might signal infection. Declining blood pressure could indicate sepsis. Increasing heart rate might suggest pain, anxiety, or cardiovascular issues.
The challenge: Vital signs are typically documented multiple times per day across hundreds of pages. They might appear in nursing flow sheets, progress notes, or dedicated vital sign logs. The critical information isn't in any single reading - it's in the trend.
What you're looking for:
- Abnormal values that weren't recognized or acted upon
- Trends suggesting deterioration that staff missed
- Gaps in monitoring for high-risk residents
- Whether abnormal vitals triggered appropriate interventions
Why manual review is hard: You're scrolling through dozens or hundreds of entries, trying to mentally track whether a resident's temperature went from 99°F to 100.1°F to 101.3°F over three days while staff documented "vital signs stable." You're looking for patterns across time that aren't visually obvious in narrative notes.
2. Laboratory Values: The Chemical Story
What it includes: Complete blood counts (CBC), comprehensive metabolic panels (CMP), albumin, prealbumin, hemoglobin, creatinine, glucose levels, urinalysis results, culture and sensitivity reports
Why it matters: Lab values tell you what's happening inside the body. Dropping albumin indicates malnutrition. Rising white blood cell counts suggest infection. Declining hemoglobin might point to anemia or internal bleeding. Abnormal creatinine levels signal kidney problems.
The challenge: Lab results come from external laboratories and are often scattered throughout the medical record. A critical value might be buried in a progress note, attached as a separate lab report, or mentioned in a physician order. Some facilities have better lab integration than others.
What you're looking for:
- Critical values that didn't trigger intervention
- Lab results that were never followed up
- Trends showing progressive malnutrition or dehydration
- Whether lab work was ordered appropriately based on symptoms
- Correlation between lab values and clinical presentation
Why manual review is hard: Lab reports use medical abbreviations and reference ranges. You need to understand not just whether a value is abnormal, but whether it's critically abnormal, and whether the facility's response was appropriate. You're often comparing values across weeks or months to identify trends.
3. Weight Trends: The Nutrition Narrative
What it includes: Weekly or monthly weight measurements, height (for BMI calculation), documentation of food/fluid intake
Why it matters: Significant weight loss is one of the clearest indicators of neglect in nursing home cases. Residents who lose 10%, 15%, or 20% of their body weight over several months are often not receiving adequate nutrition and hydration. This can lead to pressure injuries, infections, and death.
The challenge: Weights should be documented regularly, but the frequency varies by facility policy and resident acuity. Some facilities weigh residents weekly, others monthly. The weights might be in different units (pounds vs. kilograms) or documented in different locations (nursing notes, nutritional assessments, dietary logs).
What you're looking for:
- Progressive weight loss over time
- Whether significant weight loss triggered dietary interventions
- Correlation between weight loss and declining function
- Whether the facility's nutritional care plan was adequate
- Documentation (or lack thereof) of food and fluid intake
Why manual review is hard: You're hunting through months of records to find weight entries, converting units if necessary, calculating percentage changes, and determining whether the facility recognized and responded to concerning trends. A 150-pound resident who drops to 130 pounds over three months has lost 13% of their body weight—that's significant. But identifying that pattern requires finding weights scattered across dozens or hundreds of pages.
4. Wound Documentation: Measuring Deterioration
What it includes: Wound measurements (length, width, depth in centimeters), stage classification (Stage 1-4 for pressure injuries), wound location, wound bed description, exudate type and amount, surrounding skin condition, photographs, treatment records
Why it matters: Pressure injuries are among the most common nursing home negligence cases. The progression from Stage 1 (non-blanchable redness) to Stage 4 (full-thickness tissue loss with exposed bone, tendon, or muscle) can indicate inadequate turning and repositioning, poor nutrition, or failure to treat developing wounds.
The challenge: Wound documentation can be incredibly detailed or frustratingly vague. Some facilities have comprehensive wound assessment forms with precise measurements and staging. Others have brief narrative notes like "pressure area noted to sacrum." Tracking how a single wound changes over time requires finding every reference to that specific wound location across weeks of documentation.
What you're looking for:
- Initial wound identification and staging
- Progression or regression of wound stage
- Changes in wound measurements over time
- Whether wounds were measured and assessed per facility policy
- Correlation between wound progression and turning/repositioning compliance
- Whether treatment was appropriate for the wound stage
- Photographic documentation (or suspicious absence thereof)
Why manual review is hard: A single resident might have multiple wounds on different body parts. You need to track each wound separately, distinguish between them in the documentation, and create a timeline showing whether each wound improved or deteriorated. Measurements might be in one section, staging in another, and treatment notes in a third. Some facilities use wound care flow sheets; others bury wound information in narrative nursing notes.
5. Turning and Repositioning Logs: The Pressure Relief Record
What it includes: Date and time of position changes, position resident was turned to (left side, right side, back, sitting), staff initials
Why it matters: Immobile residents must be turned and repositioned at least every two hours to prevent pressure injuries. Turning and repositioning logs are the facility's record that they performed this basic care. Gaps in these logs - or patterns suggesting falsification - can be strong evidence of neglect.
The challenge: These logs are often simple checkboxes or tables, but they span weeks or months. Some facilities have electronic systems; others use paper logs that get scanned into the record. The logs might be complete, might have suspicious patterns (every entry at exactly 2-hour intervals with no variation), or might have significant gaps.
What you're looking for:
- Gaps of more than 2-3 hours between position changes
- Patterns suggesting pre-charting or falsification (too perfect, no variation)
- Correlation between gaps in turning and wound development/progression
- Whether high-risk residents received more frequent turning
- Whether the facility followed its own policies
Why manual review is hard: You're looking at repetitive tabular data spanning hundreds of entries. Finding the gaps or patterns requires sustained attention. You need to correlate the timing of gaps with other events - did the pressure injury on the sacrum develop during the three-week period when turning logs show multiple 4-6 hour gaps?
6. Incident Reports and Falls Documentation: The Red Flag Events
What it includes: Fall incident reports, injury reports, descriptions of what happened, witness statements, immediate interventions, notification of family/physician
Why it matters: Falls are leading causes of injury and death in nursing homes. But not every fall is the facility's fault. You need to understand: Was the resident assessed as a fall risk? Were appropriate interventions implemented? How did the fall happen? Was there a witness? What injuries resulted? How quickly was the resident evaluated?
The challenge: Incident reports might be in a separate section, or they might not be produced at all (facilities sometimes claim they're "not medical records"). Fall documentation might appear in nursing notes, physician orders, or therapy assessments. A single fall might generate documentation in multiple locations—or surprisingly little documentation at all.
What you're looking for:
- Fall risk assessments and whether the resident was identified as high-risk
- What interventions were in place (bed alarms, low bed, fall mat, etc.)
- Whether those interventions were actually used
- Description of how the fall occurred
- Whether the fall was witnessed or unwitnessed
- Injuries sustained and whether resident was sent to hospital
- Multiple falls over time (patterns)
- Whether fall interventions were updated after each fall
Why manual review is hard: You need to piece together information from multiple sources to understand a single fall event. Then you need to track multiple falls over time and assess whether the facility's response evolved appropriately. You're correlating fall documentation with care plans, risk assessments, and safety interventions.
7. Medication Administration Records (MARs): The Timing and Compliance Picture
What it includes: Medication name, dose, route, frequency, scheduled administration times, actual administration times, staff initials, held or refused medications with reasons
Why it matters: Medication errors can be deadly. Residents who don't receive antibiotics for infections, pain medications for comfort, or anticoagulants for stroke prevention can suffer serious harm. But proving a medication error requires showing that medications were delayed, omitted, or given incorrectly.
The challenge: MARs are dense, tabular documents covering every medication a resident takes. A single resident might be on 10-15 medications, each with different schedules. The MAR might span months and hundreds of pages. Identifying gaps, delays, or patterns of missed medications requires careful review.
What you're looking for:
- Medications that were ordered but not administered
- Delays in administration (medication due at 9 AM but given at 2 PM)
- Patterns of missed doses for critical medications
- Correlation between missed medications and resident deterioration
- PRN (as needed) pain medications that were requested but not given
- Medication orders that weren't transcribed to the MAR
- Suspicious patterns (medications marked as "refused" repeatedly)
Why manual review is hard: MARs are spreadsheet-like documents with rows for each medication and columns for each day/time. Finding gaps requires scanning hundreds of cells. You need to understand which missed medications are critical versus less important. You're looking for patterns - not a sin gle missed dose, but repeated failures to administer important medications.
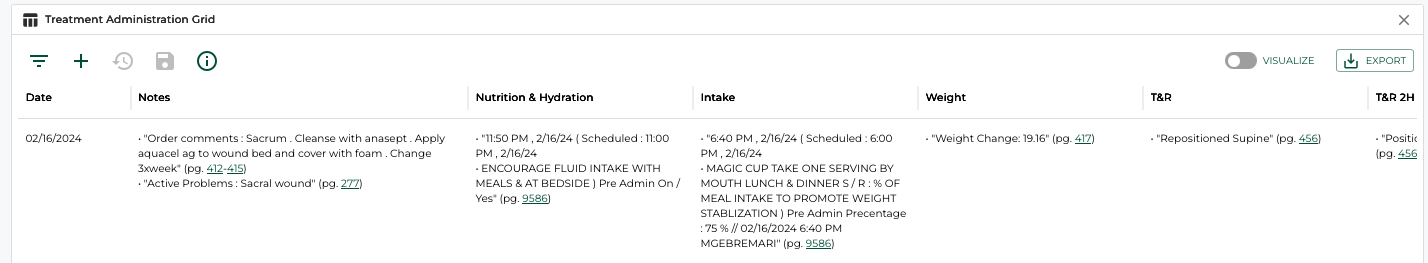
The Real Challenge: Correlation Across Data Streams
Here's what makes nursing home cases uniquely complex: None of these data streams tell the full story on their own.
Consider a pressure injury case:
- Weight trends show the resident lost 18% of body weight over 4 months
- Lab values show declining albumin and prealbumin (malnutrition markers)
- Wound documentation shows a Stage 2 sacral pressure injury first noted on March 15 that progressed to Stage 4 by May 1
- Turning and repositioning logs show multiple 6-8 hour gaps in March and April
- Vital signs show increasing temperature in late April (infection)
- Lab values show elevated WBC count in late April (confirming infection)
- Medication records show antibiotics ordered April 28 but first dose not given until April 30
The negligence isn't visible in any single data stream. It's in the correlation:
- The facility didn't recognize or address progressive malnutrition (weight + labs)
- The malnutrition contributed to pressure injury development (correlation)
- The facility failed to turn the resident adequately (turning logs)
- The pressure injury progressed from Stage 2 to Stage 4 in 6 weeks (wound docs)
- The wound became infected (vitals + labs)
- The facility delayed antibiotic administration (MARs)
Creating this timeline manually takes hours or days. You're flipping between different sections of the record, making notes, creating spreadsheets, and trying to hold multiple data streams in your mind simultaneously.
And this is for a single issue - a pressure injury. Many nursing home cases involve multiple issues: falls, infections, dehydration, medication errors, all happening concurrently or sequentially.
Why This Matters for Case Screening
Remember the brutal math of nursing home case screening: attorneys investigate 10 cases for every one they take. That means nine times out of ten, after hours or days of this detailed review, the conclusion is "we can't prove causation" or "the injuries were primarily from the resident's underlying conditions."
This is why nursing home case screening is so resource-intensive. And this is why attorneys desperately need technology that can:
- Extract structured data from semi-structured documents (pulling weights from various note types into a single trend line)
- Normalize data across different formats and units (converting weights to consistent units, standardizing wound measurements)
- Visualize trends over time (showing weight loss graphically rather than as scattered numbers in notes)
- Correlate across data streams (identifying when wound progression coincided with gaps in turning)
- Flag patterns of concern (highlighting when abnormal vitals weren't followed up)
- Generate timelines (creating a chronological view of events across all seven data streams)
Generic AI tools aren't built for this. They can summarize individual documents, but they can't extract structured data from semi-structured formats. They can answer questions about content, but they can't identify patterns across hundreds of pages. They can create chronologies, but they miss the medical significance of trends.
Nursing home cases require purpose-built technology that understands these seven data streams and, more importantly, how to correlate them.

What Attorneys Actually Need
In conversations with experienced nursing home litigators, they consistently describe needing the same things:
"I need to see vital signs and labs over time - not individual values, but trends."
"I need to know if there are gaps in the turning logs that correlate with when the pressure injury developed."
"I need to see weight progression and whether the facility responded when the resident lost significant weight."
"I need to understand whether medication timing issues contributed to the outcome."
"I need all of this in hours, not days, so I can make screening decisions efficiently."
This isn't about replacing attorney judgment. The attorney still decides whether the facility's care fell below the standard, whether causation can be proven, and whether the case is worth pursuing.
But the preliminary work - extracting these seven data streams, creating timelines, identifying patterns, and flagging potential issues - can and should be automated.
The Path Forward
At Parambil, we're building AI specifically designed for nursing home case analysis. Our technology understands these seven data streams, knows where to find them in complex medical records, and can correlate them to create the comprehensive picture attorneys need.
We're not trying to replace the expertise of experienced nursing home litigators. We're trying to give them back their time - and to make it feasible for more attorneys to take on this challenging but crucial work.
Because at the end of the day, every case that goes unexamined due to resource constraints is a vulnerable resident who didn't get justice - and a facility that didn't face accountability.
Want to see how AI can accelerate your nursing home case analysis?
We're hosting an exclusive webinar where we'll demonstrate our purpose-built solution for nursing home litigation and gather feedback from experts in the field.
Whether you're drowning in case screening, looking to expand your nursing home practice, or simply curious about how technology can help with these complex cases, we'd love to hear from you.
Sign up for our upcoming webinar.
Let's build the future of nursing home litigation together - one that makes justice more accessible and protects more vulnerable residents.



